How a Healthy Gut Microbiome May Support Neuroplastic Pain, Fibromyalgia and ME/CFS
Claire Rice
1/12/20262 min read
How a Healthy Gut Microbiome May Support Neuroplastic Pain, Fibromyalgia and ME/CFS
Chronic pain and fatigue conditions such as neuroplastic (nociplastic) pain, fibromyalgia, and ME/CFS are increasingly understood as disorders of nervous system regulation, immune signalling, and energy metabolism — not simply problems within muscles or joints.
One area of growing interest is the gut microbiome: the trillions of bacteria, viruses, and fungi living in the digestive tract. While research is still evolving, there is a strong and biologically plausible case that supporting a healthy microbiome may play a meaningful role in symptom management.
Understanding Neuroplastic Pain, Fibromyalgia and ME/CFS
These conditions share several core features:
Central sensitisation – an overactive nervous system that amplifies pain and sensory signals
Immune dysregulation and low-grade inflammation
Autonomic nervous system imbalance (fight-or-flight dominance)
Fatigue, brain fog, sleep disturbance and gut symptoms
Crucially, this does not mean symptoms are “all in the mind”. It means the brain, nerves, immune system and metabolism are interacting differently — and the gut sits at the centre of that interaction.
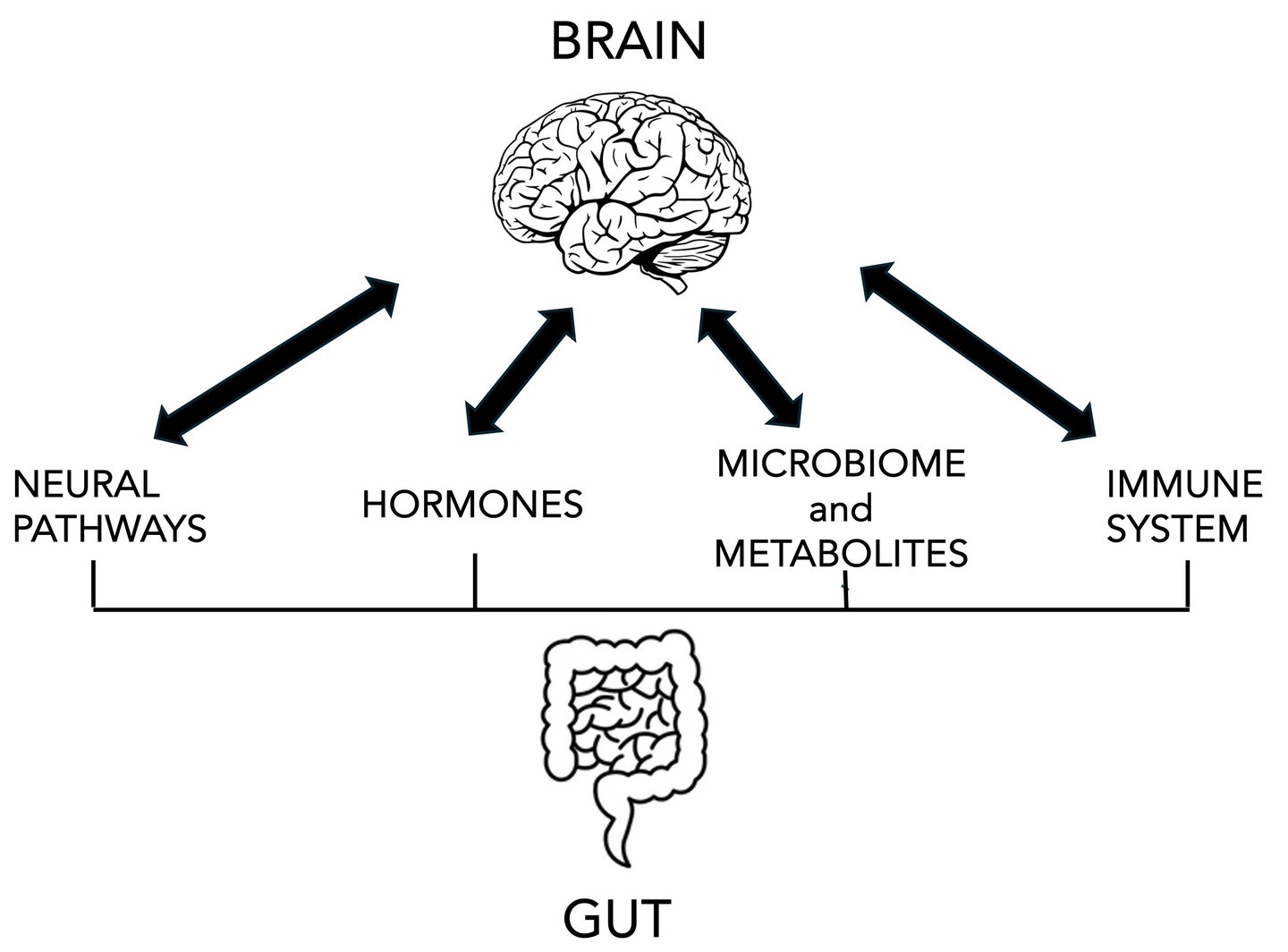
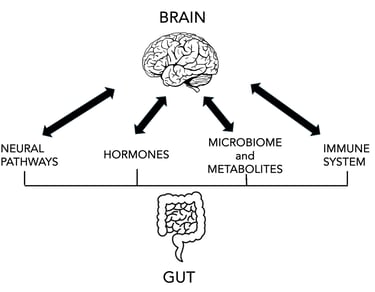
The Gut–Brain–Immune Axis
The gut communicates constantly with the brain and immune system via:
The vagus nerve
Immune signalling molecules (cytokines)
Microbial metabolites such as short-chain fatty acids (SCFAs)
Hormones and neurotransmitters (including serotonin and GABA)
A disrupted microbiome (dysbiosis) can increase intestinal permeability (“leaky gut”), allowing inflammatory signals to circulate — potentially fueling pain sensitisation and fatigue.
Why the Microbiome Matters in Neuroplastic Pain
Neuroplastic or nociplastic pain arises when pain pathways become over-learned and hyper-reactive, even in the absence of ongoing tissue damage.
A healthy microbiome may help by:
Reducing neuroinflammation
Supporting vagal tone, helping the nervous system shift out of threat mode
Producing SCFAs (especially butyrate) that help regulate microglial activation in the brain
Influencing neurotransmitters involved in pain modulation
Animal models consistently show that altering the gut microbiome can increase or reduce pain sensitivity — one of the strongest signals in this field.
Fibromyalgia and the Microbiome
People with fibromyalgia frequently report:
IBS-type symptoms
Food sensitivities
Bloating and altered bowel habits
Research has identified distinct differences in gut bacterial composition in fibromyalgia compared with healthy controls. While this does not yet prove causation, it supports the idea that the microbiome may be involved in:
Pain amplification
Fatigue
Cognitive symptoms (“fibro fog”)
Small human studies (including dietary and microbiome-targeted interventions) suggest symptom improvements are possible, but larger, better-controlled trials are still needed.
ME/CFS, Energy Metabolism and the Gut
ME/CFS is characterised by:
Profound fatigue
Post-exertional symptom exacerbation
Immune and autonomic dysfunction
The microbiome may be relevant through its effects on:
Mitochondrial function and energy production
Immune balance
Gut barrier integrity and endotoxin exposure
Several studies show reduced microbial diversity and altered metabolic outputs in ME/CFS. Again, this doesn’t yet mean the microbiome is the cause — but it may be a modifiable contributor.
What Does the Evidence Say Overall?
Strength of evidence by area:
Biological plausibility: Strong
Animal and mechanistic studies: Strong
Human observational studies: Moderate
Human intervention trials (diet, probiotics, FMT): Early and mixed
In other words:
👉 Promising, sensible to support — but not a standalone cure.
Supporting a Healthy Microbiome (Safely)
For people with chronic pain and fatigue, the goal is gentle support, not aggressive intervention.
Helpful strategies may include:
A diverse, fibre-rich, anti-inflammatory diet (as tolerated)
Polyphenol-rich foods (berries, olive oil, herbs, colourful plants)
Identifying and addressing individual food intolerances
Supporting gut regularity and digestive comfort
Cautious, personalised use of prebiotics or probiotics
Avoiding unnecessary restriction, which can reduce microbial diversity
Any intervention should be paced and personalised, particularly in ME/CFS where symptom flares can occur.
The Take-Home Message
A healthy microbiome won’t “switch off” neuroplastic pain, fibromyalgia or ME/CFS on its own — but it may:
Lower inflammatory load
Improve nervous system regulation
Support energy metabolism
Enhance resilience to stressors
As part of a whole-person, systems-based approach, microbiome support is a low-risk, potentially high-impact foundation for many people living with chronic pain and fatigue.
Get in touch
Subscribe to the mailing list (your details will not be shared)
GPhC registration, Claire Rice 2082362
The Coaching Pharmacist Ltd Company number 16802064 registered in England
